Seasonal allergies can make motherhood feel even more exhausting. Between sneezing, congestion, itchy eyes, and sinus pressure, many breastfeeding mothers wonder if they can safely take allergy me...

Prior To First Use Do not wash/sterilize the tubing(s). They will never come into contact with breast milk since Spectra pumps are closed-system pumps. Wash all other parts in warm soapy water, ...

Whether you’re returning to the office, working a hybrid schedule, or logging in from home, you can continue breastfeeding and maintain a healthy milk supply.

Jenn Foster, IBCLC With the passing of the Affordable Care Act (ACA), insurance companies now MUST cover a breast pump for mothers during their pregnancies. This includes Medicaid and Medicare. The...

Holidays are full of travel, family, and fun—but let’s be honest, keeping up with your pumping routine can be a challenge. With a little planning and the right tools, you can maintain your milk sup...

If you have been researching breast pumps, the terms “primary pump” and “secondary pump” come up a lot — but what do they really mean? A primary breast pump is a tabletop pump designed for frequ...
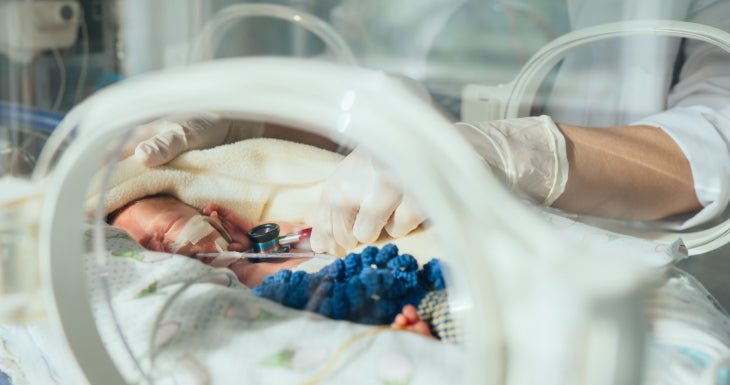
As a parent with a baby in the NICU, you’re likely navigating a lot of emotions, and in addition to caring for your baby, you’re focused on establishing a solid breastfeeding routine. One of the mo...

For many moms, wearable pumps have become a total game-changer—offering the freedom to pump while holding your baby, managing a jam-packed schedule, or simply taking a moment to relax and enjoy som...

If you’ve come across this article, chances are you’re deep in the newborn trenches—navigating life with a brand-new baby, adjusting to your growing family, and figuring out everything in between. ...

5 tips to prep for your time away from home New moms, we know travel can be tough. Not only do you have to spend time away from your little one, but you also have to worry about how, when, and whe...

by Bonne Dunham, IBCLC Pumping Milk…Am I Doing It Right? First of all, there are A LOT of right ways to do it! Pumping is a learned activity that gets easier with time and practice. At first, most ...

Travel Tips for Flying While Pregnant Whether you’re traveling for work or pleasure, now that you are pregnant you may be wondering what steps and precautions you should be taking. Since pregnancy ...

Every year, on January 27th, we celebrate World Pumping Day, a global event dedicated to recognizing and empowering parents who pump breast milk. This day shines a spotlight on the effort, love, an...


